Deep vein thrombosis (DVT) can be a worry for frequent travellers. It occurs when altered blood flow leads to the formation of a blood clot in a deep vein of the leg. Symptoms include a swollen or painful calf or thigh. In uncommon cases, part of the clot moves to the lungs, causing a pulmonary embolism (blocked blood vessel) that, if severe, may cause the affected lung to collapse.
DVT isn’t caused only by travelling. Each year it occurs in between one and three people per 1,000, according to the UK Department of Health, and, of those, only one in 100 cases is fatal. Nevertheless, frequent travellers are probably more at risk than others. Why is that? Professor Mark Whiteley, a consultant venous surgeon and phlebologist explains:
“The things that cause clots are the Virchow’s Triad [named after German physician Rudolf Virchow]. These are changes in the blood, changes in the blood flow and changes in the vessel wall. Any one of those can cause a clot.
“When you fly, you have a change in the flow, since you’re just sitting there, so the blood isn’t flowing as it should. You’re up in the air, so you have decreased oxygen and have changed the consistency of the blood. Finally, if you have varicose veins, then the vein wall is stretched and bulbous allowing blood to clot on this altered vein wall. So when you fly, you’ve got the perfect storm for DVT.”
For quick advice on that, see our article:
Our previous article dealt with some of the practical ways of guarding against DVT such as staying hydrated, keeping moving when on the plane and wearing compression socks. The publicity around these measures has probably saved many people who would have suffered from DVT from having serious problems. There’s no doubt, though, that some of us are more at risk than others, and so if you have varicose veins, it would be an idea to see a specialist.
Whiteley points out that significant proportion of the population are unaware that they have varicose veins, as not all are visible on the surface.
“Venous disease affects around 30-40 per cent of people, and of that 30-40 percent, only 15-20 percent of people know they have got problems with their veins, because they can see them. The others are hidden under the skin’s surface.
“Yet whether they are visible or not, most vein disease will cause aching and painful legs and can lead to swollen ankles and ultimately, it can go on to cause leg ulcers and clots. Yet even in those cases, if you go to the doctor you will often be given leg stockings or steroid treatments, neither of which really work because they don’t fix the underlying problem.”
For those people who do have veins that show, who have suffered from leg ulcers or superficial vein thrombosis (“phlebitis”), or who have a family history that might indicate problems are likely, Whiteley recommends having a peremptory scan.
Since my varicose vein shows, I thought it worth at least having the scan. My attitude towards undergoing surgery are that I have successfully avoided it all my life, and I intend to continue doing so. Nevertheless, a scan isn’t painful, and at least then I could make an informed decision. So it was that I found myself having an initial consultation with Whiteley at his clinic just off London’s Oxford Street (he also runs clinics in Guildford and Bristol).
The scans performed by a highly trained technologist were extremely thorough, but then in many ways they are the most important part of the treatment. The scan should ensure that every problematic vein, whether visible or not, is identified, and also help the surgeon decide on what sort of treatment will be appropriate.
The Duplex scanning technique used is, in fact, a three-fold process (it’s actually called ‘triplex scanning’ in some parts of the world). It starts with a greyscale/B-mode ultrasound scan similar to the standard sort of ultrasound scan used for pregnancy.
Then there is a ‘Doppler ultrasound’ scan, beamed into the specific area of the body and capable of being directed inside the vein. By combining the ultrasound picture generated with the specific Doppler waveform, Doppler ultrasound can be used to measure blood flow in the vein.

“The third part of the scanning process is the ‘colour flow’/‘colour-coded’ element,” explains Whiteley. “Computers these days are so fast that any movement on the black and white ultrasound picture can be picked up and ‘coded’ as either blue or red depending on the direction of flow. This mean we can see blood flow in a vein in real time and judge whether blood flows up the vein normally and down abnormally, if the valves are not working.”
All of this is then brought together so that a completely bespoke treatment can be suggested to the patient. In my case, apart from some aching, the vein had never bothered me, but the scans showed that as well as the visible vein, there were other deeper problems. Of course, as with all medical matters, the moment you are told something affects you, then it’s time to start researching, initially on Google, then ringing friends who have absolutely no specialism in the area you are asking about, but who try to be helpful, and finally listening to the specialist in front of you.
“In the UK, we get taught that there are only two layers of veins: deep in the muscle and superficial,” says Whiteley. “So it’s generally understood that if you have a clot in the deep veins, that’s bad because it can go to the lungs, and if you get a lump in the superficial, you don’t need to worry, because it’s just painful, and most doctors just give antibiotics.”
This was interesting, because it is exactly what has happened to a frequent-travelling colleague of mine, who has twice suffered from a painful lump just underneath the skin after flying long haul. The first time he was prescribed antibiotics, the second time a scan and some anti-coagulants.
“If something is hot and red, doctors tend to reach for antibiotics,” says Whiteley. “But if you got punched in the nose it would be hot and red, but you wouldn’t give antibiotics. It is the irritation of the clot which causes a hot red area because the body is trying to heal.
“Instead, there are two things that should be done. The latest guidance from the British Committee for Standards in Haematology and the American College of Chest Physicians Evidence-Based Clinical Practice Guidelines since 2012 is to come and have a scan. What we know is that if that clot is within five centimetres of a junction to the deep vein, it can turn into a DVT.”
Worryingly, Whiteley says that these guidelines show that around one per cent of people who have a clot in the superficial veins that is close to the junction end up with a clot in their lungs. “Yet doctors are still giving non-steroidal anti-inflammatories and aspirin to patients and telling them to put a stocking on. If it’s close to a deep vein they must get a scan and then be offered anti-coagulant.”
(I have advised my colleague to go for a scan. We shall see.)
So what was the advice? Would it be necessary to have the veins removed (or stripped, as I’ve heard it called, normally with a wince)?
Thankfully not.
“In the UK, we still have some people having their veins stripped out, but it’s pointless because they almost always grow back, and grow back without valves, which means the problem has returned,” says Whiteley.
“We did a study showing that at eight years, 82 per cent who had their veins stripped have grown their veins back again. The latest research shows you also get smaller new veins developing as well making it more difficult to treat.”
Whiteley says that instead, it is better to destroy the veins with heat directed at the vein wall, so the cells undergo a process called apoptosis. The trick is to use a combination of techniques. In the past, radiofrequency ablation was used, but that only treated the vein it was touching. Therefore if the vein wall bulged away from the radiofrequency device, or there was a clot or scar in the vein stopping it from being in contact during the treatment, then treatment could fail.
Most treatment now is by laser, but Whiteley says that “saying “laser” is like saying “car”. There are many different types of laser, just as there are many different sort of car.” Sonovein is completely different and is the latest technique to treat veins. This beams ultrasound in a cone-shape through the skin, and only burns tissue at the focus of the cone.
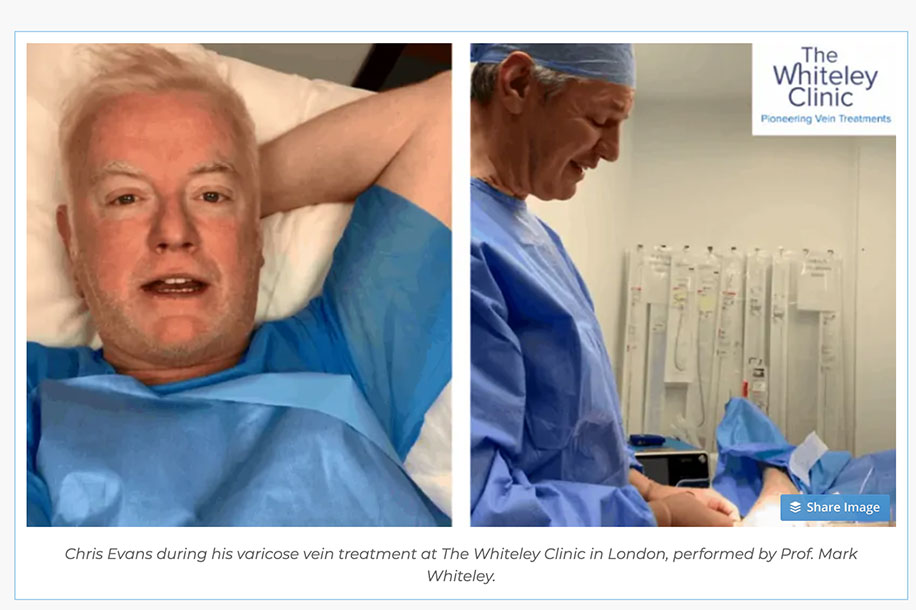
Unfortunately, my veins were too extensive and long. For this treatment. So I had another new treatment called microwave ablation. This is the same new technique that Whiteley used on the DJ Chris Evans last year, that Evans showed off in the press.
So once the correct combination of techniques was decided on, it was time to book the day for the treatment. In fact, it only took an hour, and was done under a local anaesthetic. While this was uncomfortable, being awake is necessary, so you can advise on levels of discomfort as the microwave kills off veins. By being able to feedback to the surgeon, it prevents overheating and burns. This protects the skin and nerves and is why modern vein experts never use general anaesthetic or sedation.
Afterwards, my leg was encased in tight bandages, and I rested for 30 minutes before walking out of the surgery, into a waiting Uber and off to the train station and home. Three days later the bandages were off, and I could see a transformed, if heavily bruised leg. Twelve weeks later I was back and ready for the next stage of the treatment – foam.
“Once your leg has had the veins removed, there are only three reasons you should get the vein back. Firstly, you haven’t had the right ones treated, secondly, you had the right veins treated but with the wrong technique, so maybe laser but the wrong power, and finally new veins have opened up. This last part can be reduced by foam sclerotherapy.”
Ultrasound-guided foam sclerotherapy is used because any bulging surface veins that have been removed during the procedure will try to re-grow again. The foam stops them growing back.
Thankfully, the foam procedure was not painful at all, and took less than an hour. My leg was then wrapped tightly in bandages, and a long stocking put over them. The trick then was to keep the leg wrapped up for three weeks, which was irritating for the first day or so, but soon seemed normal.
During this time, I took several long-haul flights, including a week-long trip to Hong Kong, and suffered no ill effects. In fact, I just made sure to put a stocking on the other leg, for safety’s sake, even though there are no problematic veins on that one. For showering there was a long plastic cover, eponymously called a Limbo, which was very effective. Finally, after three weeks, there was the unveiling of my new leg, free of varicose veins, and ready to take its place in the world of short trousers without any unsightly bulges.
This combination of vanity and concern for health could be life-saving, according to Professor Christopher Ogden, a consultant uro-oncologist and pioneer of robotic surgery in the UK, who attended a recent Business Traveller event at London’s Cromwell Hospital.
Business Traveller readers’ event at London’s Bupa Cromwell Hospital
He advises prioritising mental health up until the age of 50 and thereafter concentrating on physical health, with health screenings for cardiovascular disease and cancers of the prostate and colon. For those suffering from painful veins, especially those who travel frequently, I would advise having a general MOT to discover potential problems, and considering having them fixed. With luck, we are looking at longer lives, and treatments such as those for varicose veins can help ensure a more comfortable duration.